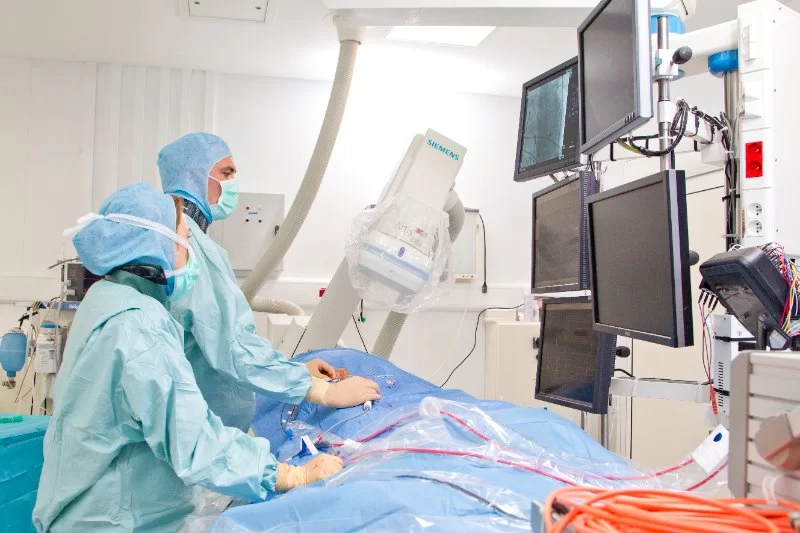
What Is Cardiac Ablation?
Cardiac ablation is a medical procedure used to treat arrhythmias—irregular heartbeats that can lead to serious health issues. It involves using catheters and energy sources such as radiofrequency (RF) energy or cryotherapy to destroy small areas of heart tissue that are causing the abnormal electrical signals responsible for the arrhythmia. But what does the procedure entail, and why is it necessary? Let’s dive into the details.
How Cardiac Ablation Works
Cardiac ablation is typically performed in a hospital setting by a specialized cardiologist known as an electrophysiologist. The procedure starts with the insertion of catheters through blood vessels in the groin or neck. These catheters are then guided to the heart, where they are used to map the electrical activity of the heart. Once the abnormal signals are located, the physician will use either RF energy or freezing techniques to destroy the tissue causing the irregular heartbeat.
Radiofrequency Energy
Radiofrequency energy is the most commonly used method. It involves sending high-frequency electrical energy through the catheter to heat and destroy the tissue responsible for the arrhythmia. This is often referred to as "burning" the tissue.
Cryotherapy
In some cases, doctors may use cryotherapy, which involves freezing the problematic tissue to stop the abnormal signals from spreading. This is typically used in specific types of arrhythmias, like atrial fibrillation (AFib).
Who Needs Cardiac Ablation?
Cardiac ablation is recommended for individuals who suffer from arrhythmias that cannot be managed with medications or lifestyle changes alone. Arrhythmias occur when the heart’s electrical system malfunctions, leading to too fast, too slow, or irregular heartbeats. These irregularities can be dangerous, causing symptoms like dizziness, fainting, fatigue, and, in some cases, more severe complications like stroke or heart failure.
Types of Arrhythmias Treated with Cardiac Ablation
The most common types of arrhythmias that may require ablation include:
- Atrial Fibrillation (AFib): The most common heart arrhythmia, AFib causes the heart’s upper chambers to quiver instead of contracting normally, which can lead to blood clots, stroke, and heart failure.
- Atrial Flutter: A condition that causes the heart to beat too fast, often leading to symptoms like palpitations and dizziness.
- Supraventricular Tachycardia (SVT): An abnormally fast heart rhythm originating above the heart’s ventricles.
- Ventricular Tachycardia (VT): A rapid heartbeat originating from the lower chambers of the heart, which can be life-threatening if left untreated.
When Is Cardiac Ablation Recommended?
Cardiac ablation may be recommended when:
- The arrhythmia is severe and causing significant symptoms like dizziness, fainting, or shortness of breath.
- Medications are not effective or cause side effects.
- The arrhythmia is putting you at risk for more serious conditions, such as stroke or heart failure.
- Other non-invasive treatments have not provided relief.
Benefits of Cardiac Ablation
One of the primary benefits of cardiac ablation is the potential for long-term relief from arrhythmias, often leading to a better quality of life. Here are some additional benefits:
1. Improved Heart Function
By eliminating the abnormal electrical signals, ablation helps restore the heart’s normal rhythm, allowing it to pump more effectively. This can reduce symptoms like fatigue, shortness of breath, and dizziness.
2. Reduced Risk of Stroke
In conditions like atrial fibrillation, blood can pool in the heart and form clots, which may travel to the brain and cause a stroke. By addressing the underlying arrhythmia, cardiac ablation lowers the risk of clot formation and stroke.
3. Reduced Dependence on Medication
Many patients experience a reduction in the need for anti-arrhythmic medications after undergoing ablation. This can lead to fewer side effects and a simpler treatment regimen.
Risks and Considerations
While cardiac ablation is generally safe, like any medical procedure, it does come with risks. Potential complications include:
- Bleeding or infection at the catheter insertion site
- Damage to the heart’s blood vessels or valves
- Perforation of the heart wall
- Arrhythmias that may require additional treatment
It’s essential to discuss these risks with your doctor and understand the potential benefits and drawbacks before deciding to proceed with the procedure.
How to Prepare for Cardiac Ablation
Before the procedure, your doctor will conduct a thorough evaluation to assess your heart health. This may include blood tests, an electrocardiogram (ECG), or other imaging tests. You may be asked to stop taking certain medications that could affect the procedure, such as blood thinners, and refrain from eating or drinking for a certain period before the procedure.
Recovery After Cardiac Ablation
The recovery time for cardiac ablation varies depending on the individual and the extent of the procedure. In most cases, patients can go home the same day or the following day. It’s common to experience some soreness or bruising at the catheter insertion sites, but this usually subsides within a few days.
Most people can return to normal activities within a few days to a week, but it’s essential to avoid strenuous activities for a few weeks while your heart heals. Your doctor will provide specific instructions for post-procedure care.
Final Thoughts
Cardiac ablation is a highly effective procedure for treating a variety of arrhythmias, offering relief for patients who have not found success with medications alone. If you or a loved one suffers from an arrhythmia and are considering cardiac ablation, it’s important to consult with a qualified cardiologist who can help determine the best course of action based on your specific condition.
For more information or to schedule a consultation with a heart specialist, visit HeartCare Hub for expert advice and resources.